I Was 25 Dying and They Told Me We’ve Tried Everything—David Fajgenbaum’s Fight to Cure Himself and Expose a Broken System
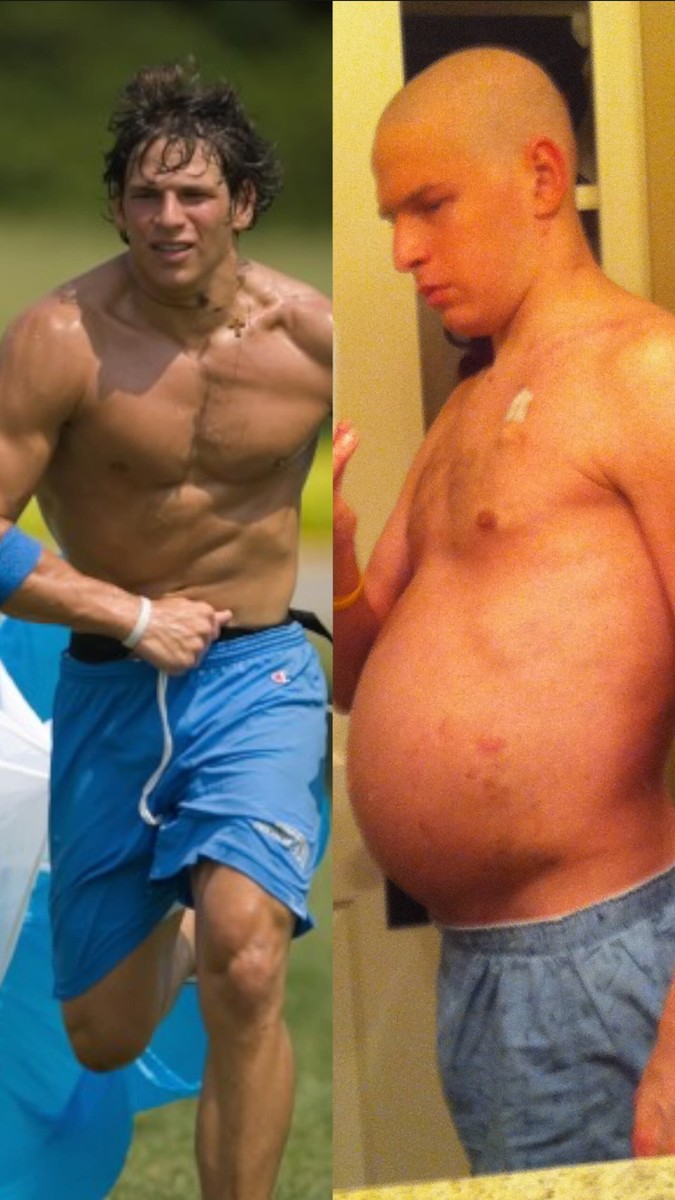
The Final Pronouncement: Doctors Tell David There’s Nothing More They Can Do In 2010, at 25 years old, David Fajgenbaum is lying in a hospital bed watching his body shut down. Not metaphorically. Literally—organ by organ. Doctors walk into his room and deliver the sentence that ends hope without drama, without comfort, without “let’s try one more thing”: “David, we’ve tried everything. There’s nothing more we can do.” At first, he barely processes it. He understands what it means only when his family walks in. Only when they start hugging him the way people hug you when they think it’s the last time. Only when a priest comes to read him last rites. And the irony cuts deeper than the illness itself: David isn’t just any patient. He’s a medical student. A former college quarterback. A young man who decided to become a doctor after his mother died of cancer. He built his life around medicine—only to end up dying from a disease he admits he’d never even heard about in medical school: Castleman disease. A rare, brutal inflammatory disorder where the immune system—often for reasons no one can clearly explain—turns on the body and starts extinguishing vital organs. No approved therapies. No real roadmap. No cure. Just collapse. At that moment, the medical team reaches for the last desperate move: a combination of seven chemotherapy drugs—not because they’re designed for Castleman disease, but because there’s nothing else left. Seven chemotherapies as a blind punch into the dark. And then something close to a miracle happens. “Amazingly, they worked,” he says. He survives. He returns to school. He continues his life. Later he even makes what he jokes might be “the worst before-and-after photo of all time”—the kind meant to inspire, except in his case it’s proof of how brutally the disease can crush a human body. The room laughs. But David’s story isn’t a comedy. Because then the disease comes back. And again. And again. Five times in three years, he “nearly dies” from the same illness. Five times. Three years. That isn’t “a battle.” That’s a loop of scheduled executions that somehow keep getting postponed. During the third relapse, the scene turns almost unbearable: David is in bed, his girlfriend Caitlin beside him, his family close, and his hospital gown is “soaked with tears.” He isn’t only crying because he’s dying again. He’s crying because he can see—clearly, violently—what will be stolen if he doesn’t survive this time: The family he’ll never have with Caitlin. The patients he’ll never treat. The cures he’ll never discover in memory of his mother. Up to that point, he’d waited. He’d hoped. Somewhere, someone in a lab would figure out a therapy in time. But then he hits the realization that changes everything: “Hope alone isn’t enough.” That’s the pivot. If he wants a chance, he can’t just lie there and pray for science to arrive. He has to go after it himself. He has to turn from a patient who waits into a patient who hunts. Except there’s one problem that destroys the romantic version of that idea: developing a new drug from scratch takes the system “15 years and a billion dollars.” He doesn’t have 15 years. He has months, maybe less, and a body that’s failing. So he locks onto the only strategy that can move at the speed of a dying person: If those seven chemotherapies saved him—even though none were made for his disease—then maybe somewhere out there is another drug, built for another illness, that can be repurposed to save him. Drug repurposing. It’s not a new concept. He reaches for the example nearly everyone knows: Viagra. Originally developed for heart problems, then repurposed for something entirely different. And later repurposed again—used today for a rare pediatric lung condition. Then he brings up thalidomide: infamous for causing horrific birth defects, later repurposed and used for leprosy and multiple myeloma. Why is repurposing possible at all? Because diseases that look completely different on the surface can share the same underlying biological mechanisms. If the same pathway is broken in two different illnesses, the same drug may be able to shut it down—or correct it—in both. And then he drops a fact that most non-doctors don’t know, but once you hear it, it rewires the whole conversation: Doctors can prescribe any FDA-approved drug for any disease if they believe the potential benefit outweighs the risk. That’s called “off-label” prescribing. This isn’t some fringe workaround. He says: “one in four prescriptions” in the United States is off-label. One in four. Every day. So he does the most extreme version of what he’s talking about. He begins studying his own blood in a lab, trying to identify a drug that already exists—something that can calm the immune chaos that’s killing him. He discovers that one “communication line” in his immune system is amplified far beyond normal. And he finds that an old transplant drug—used for decades—might be able to shut that line down. That drug has never been used for Castleman disease. But he doesn’t have options. And then he says the sentence that sounds like scientific courage and raw desperation at the same time: “I started testing it on myself.” Sirolimus. In the three years before sirolimus, he nearly died five times. After starting it, he’s been in remission for more than 11 years. Eleven. The room applauds. People cheer.
In This Article:
Relapse, Resolve, and the Moment Hope Wasn’t Enough
Five Relapses in Three Years: The Moment He Realized Hope Alone Wasn’t Enough For a moment, it feels like the end of the story. But then the disease comes back. And again. And again. Five times in three years, he “nearly dies” from the same illness. Five times. Three years. That isn’t “a battle.” That’s a loop of scheduled executions that somehow keep getting postponed. During the third relapse, the scene turns almost unbearable: David is in bed, his girlfriend Caitlin beside him, his family close, and his hospital gown is “soaked with tears.” He isn’t only crying because he’s dying again. He’s crying because he can see—clearly, violently—what will be stolen if he doesn’t survive this time: The family he’ll never have with Caitlin. The patients he’ll never treat. The cures he’ll never discover in memory of his mother. Up to that point, he’d waited. He’d hoped. Somewhere, someone in a lab would figure out a therapy in time. But then he hits the realization that changes everything: “Hope alone isn’t enough.” That’s the pivot. If he wants a chance, he can’t just lie there and pray for science to arrive. He has to go after it himself. He has to turn from a patient who waits into a patient who hunts. Except there’s one problem that destroys the romantic version of that idea: developing a new drug from scratch takes the system “15 years and a billion dollars.” He doesn’t have 15 years. He has months, maybe less, and a body that’s failing. So he locks onto the only strategy that can move at the speed of a dying person: If those seven chemotherapies saved him—even though none were made for his disease—then maybe somewhere out there is another drug, built for another illness, that can be repurposed to save him. Drug repurposing. It’s not a new concept. He reaches for the example nearly everyone knows: Viagra. Originally developed for heart problems, then repurposed for something entirely different. And later repurposed again—used today for a rare pediatric lung condition. Then he brings up thalidomide: infamous for causing horrific birth defects, later repurposed and used for leprosy and multiple myeloma. Why is repurposing possible at all? Because diseases that look completely different on the surface can share the same underlying biological mechanisms. If the same pathway is broken in two different illnesses, the same drug may be able to shut it down—or correct it—in both. And then he drops a fact that most non-doctors don’t know, but once you hear it, it rewires the whole conversation: Doctors can prescribe any FDA-approved drug for any disease if they believe the potential benefit outweighs the risk. That’s called “off-label” prescribing. This isn’t some fringe workaround. He says: “one in four prescriptions” in the United States is off-label. One in four. Every day. So he does the most extreme version of what he’s talking about. He begins studying his own blood in a lab, trying to identify a drug that already exists—something that can calm the immune chaos that’s killing him. He discovers that one “communication line” in his immune system is amplified far beyond normal. And he finds that an old transplant drug—used for decades—might be able to shut that line down. That drug has never been used for Castleman disease. But he doesn’t have options. And then he says the sentence that sounds like scientific courage and raw desperation at the same time: “I started testing it on myself.” Sirolimus. In the three years before sirolimus, he nearly died five times. After starting it, he’s been in remission for more than 11 years. Eleven. The room applauds. People cheer.

The Every Cure Mission: A Bold Step Toward Healing Everyone, Everywhere
This is where the story pivots from one man’s survival to a systemic reform movement. After the remission, David doesn’t claim a personal miracle. He turns the experience into an indictment of the system that makes it easier to find a cure for one patient than to unlock cures for thousands. During those years in remission, he marries Caitlin. They have two children. He writes a book, Chasing My Cure, which he says is being made into a movie. He becomes a professor at the University of Pennsylvania. And instead of saying “I’m saved,” he asks the darker question: What about everyone who doesn’t have the chance—or the knowledge—or the stubbornness—to do what he did? What about everyone dying while the solution is sitting in plain sight? In 2022, he co-founds an organization called Every Cure. Its mission is brutal in its simplicity: unlock “the full potential of every drug” for “every disease” it can treat. He claims they’ve already advanced 14 repurposed treatments for multiple diseases, saving thousands of lives. But he doesn’t leave it at metrics. He names people. There’s Kylo, who—because of a repurposed bone-marrow cancer drug—was able to start her first year of nursing school. That treatment is now being studied in clinical trials. There’s Michael, who walked his son down the aisle on his wedding day after a melanoma drug was repurposed to treat Michael’s rare cancer. That approach, he says, is now used around the world for that rare cancer. And then he delivers his central argument like a blunt instrument: How many life-saving uses of existing drugs are sitting on pharmacy shelves—unused—not because the science isn’t there, but because the system has no incentive to look? He frames it with numbers that feel almost obscene: Humanity has developed around 4,000 drugs for around 4,000 diseases. But there are more than 14,000 diseases with no approved therapy. More than 14,000. That isn’t a niche gap. That’s a medical universe left blank. Then he pushes even further: “One in ten of us and our children will develop a rare disease with no approved therapy.” One in ten. In his view, this is the scandal: Many existing drugs could likely treat far more diseases—for less than one percent of the cost of developing a new drug, and far faster. So why isn’t it happening systematically? He doesn’t pretend the answer is complicated. He says it in one word: profit. “The short answer is that it’s simply not profitable to pursue a new use for an existing drug, especially for a rare disease.” And for “80% of drugs that are already generic,” clinical trials are expensive, and companies can’t realistically recoup costs through sales. So instead, the system—predictably—focuses on new drugs for profitable diseases. And he doesn’t let anyone off the hook: “No one—not NIH, not FDA, not the pharmaceutical industry—no one has taken responsibility” for systematically unlocking these hidden cures. “…until now,” he adds—marking his organization as an attempt to fill that void. This is where he introduces the weapon they’re betting on: Artificial intelligence. Every Cure uses AI, he says, to “scan across the world’s knowledge” of all 4,000 drugs and all 18,000 diseases, to find the most promising matches. He explains it with a comparison everyone gets: Netflix. Just as Netflix uses data about actors, directors, and what you’ve watched to predict what you’ll watch next, their AI uses knowledge about drugs and diseases—and how they relate—to predict which approved drug might work for a disease it was never intended to treat. Not vague AI magic, he insists. A massive filtering problem. The AI evaluates “millions of drug–disease matches,” ranks the best ones with the highest potential impact, and then they push those programs forward: labs, clinical trials, or—when evidence already exists—bringing the therapy into the light so doctors actually use it. At first, he admits, even they didn’t know how they would make this real. Or fund it. Clinical trials cost money. Then he receives an email from the TED community about The Audacious Project—an initiative that selects around ten nonprofits a year to fund bold solutions to huge problems. Just knowing it existed gave them the courage to jump. They founded the organization. They applied. They were “so hopeful” they’d be selected. They weren’t. The room laughs because he tells it like a life moment, not a PR failure. So they applied again. And “just a few months ago,” they received “transformative funding.” Additional support, he says, came from the U.S. federal agency ARPA-H. With that, he claims they’re building an AI engine meant to repurpose 15 to 25 treatments by 2030—and with more funding, “dozens, even hundreds.” Then he returns to where this whole thing started: Castleman disease. Another patient. Not David. Same terrifying diagnosis. The therapies David found for himself didn’t work for this patient. He was preparing to say goodbye to his wife and daughter. He was about to be transferred to hospice. Every Cure recommended the “number one drug” from their platform. “And amazingly, it saved his life,” David says. That patient has now been in remission for more than two years. But sometimes, David explains, it isn’t even about discovering a brand-new match. Sometimes the match already exists—buried in papers, known by a handful of specialists, never adopted widely. That’s where he shares one of the most shocking sequences in his talk: Leucovorin—an inexpensive vitamin-derived compound—has evidence suggesting it can improve speech in a subgroup of children who have antibodies against the folate receptor and can’t transport folate into the brain. He points to researcher Richard Frye, who ran the first of three randomized controlled trials showing benefit in that subgroup. Then he names a child: Mason. Three years old. Nonverbal. And then—according to David: “Within three days of starting leucovorin, he began saying his first words.” Applause. Then another child: Ryan. Five years old. “Practically nonverbal.” Never shared a full thought or feeling with his parents. Doctors told them he would “probably never” be able to express emotion. And then, “within two weeks” of leucovorin, Ryan turns to his father before work and says: “Daddy, I love you.” The room erupts. David doesn’t use it as sentimental climax. He uses it as another accusation: there is a blood test that can identify children like Mason and Ryan—and that test, he says, is still rarely used. That’s why they built Every Cure: to unlock hidden treatments and make sure they reach every patient who could benefit. He adds another story from the edge of medicine: Joseph, dying from POEMS syndrome, a rare cancer. On his 30th birthday, he was saying goodbye to his girlfriend Tara. His doctor had already tried everything he could think of. Every Cure recommended three drugs “commonly used for multiple myeloma,” because POEMS is similar. “And amazingly—they worked,” David says. Instead of planning Joseph’s funeral, Joseph and Tara are planning their wedding. And Joseph is there in the audience. By now, his thesis has turned human and brutal: This isn’t about “optimizing research.” This is about people who are saying goodbye—and then, somehow, not dying. And about a system that allows that to be accident instead of standard practice.

No Patient Should Suffer When a Life-Saving Drug Is Sitting on a Shelf
Toward the end, he lifts his eyes from individual stories and goes straight at the sentence that haunts anyone who has ever sat beside a hospital bed: How many of us have been with someone we love and heard, “We’ve tried everything. There’s nothing more we can do.” And then he asks the question that collapses the confidence of that medical finale: “What if we haven’t tried everything?” What if the solution exists for them—and for thousands, maybe millions with the same disease? What if the drug already exists—and it’s sitting on a shelf in a pharmacy? In the discussion after the talk, host Latif Nasser says what everyone is thinking: it sounds “too good to be true.” People die waiting for a cure to be discovered, but maybe the answer is something as simple—and as outrageous—as walking to the corner pharmacy and finding a drug that could help. David answers without hesitation: “That’s right.” And then he repeats the reason it doesn’t happen: “…except it simply isn’t profitable to do this.” Nasser puts it into historical context: medicine used to be “cure-alls,” then modern medicine became evidence-based, targeted, laser-focused. Is David saying we need to widen the lens again? “Exactly,” David says. He adds something that sounds like a quiet confession about how the industry works: companies often consider 15, 20, even 30 diseases for a single drug, but they have to choose one or two to focus on—while the other possibilities “get lost.” His organization exists to pull those lost possibilities out of the cracks. And when asked what an ordinary person can do, he stays practical: if you’ve ever benefited from an off-label or repurposed drug, talk about it. Trials cost money. Awareness and donations help move the work forward. But the strongest line in his closing isn’t a fundraising pitch. It’s a moral standard for a civilization that has 4,000 drugs and 18,000 diseases: No patient should suffer when a life-saving drug is “sitting on a shelf in a pharmacy.” And no one should be forced to accept “we’ve tried everything” as the end— when “everything” might still be waiting, unopened, right in front of us.


